AI-Powered Revenue Cycle Automation
Automate Your Revenue Cycle .
RCM Edge eliminates manual billing workflows with real-time AI automation — reducing AR days, preventing denials, and accelerating cash flow for healthcare organizations.
Full RCM Automation Suit
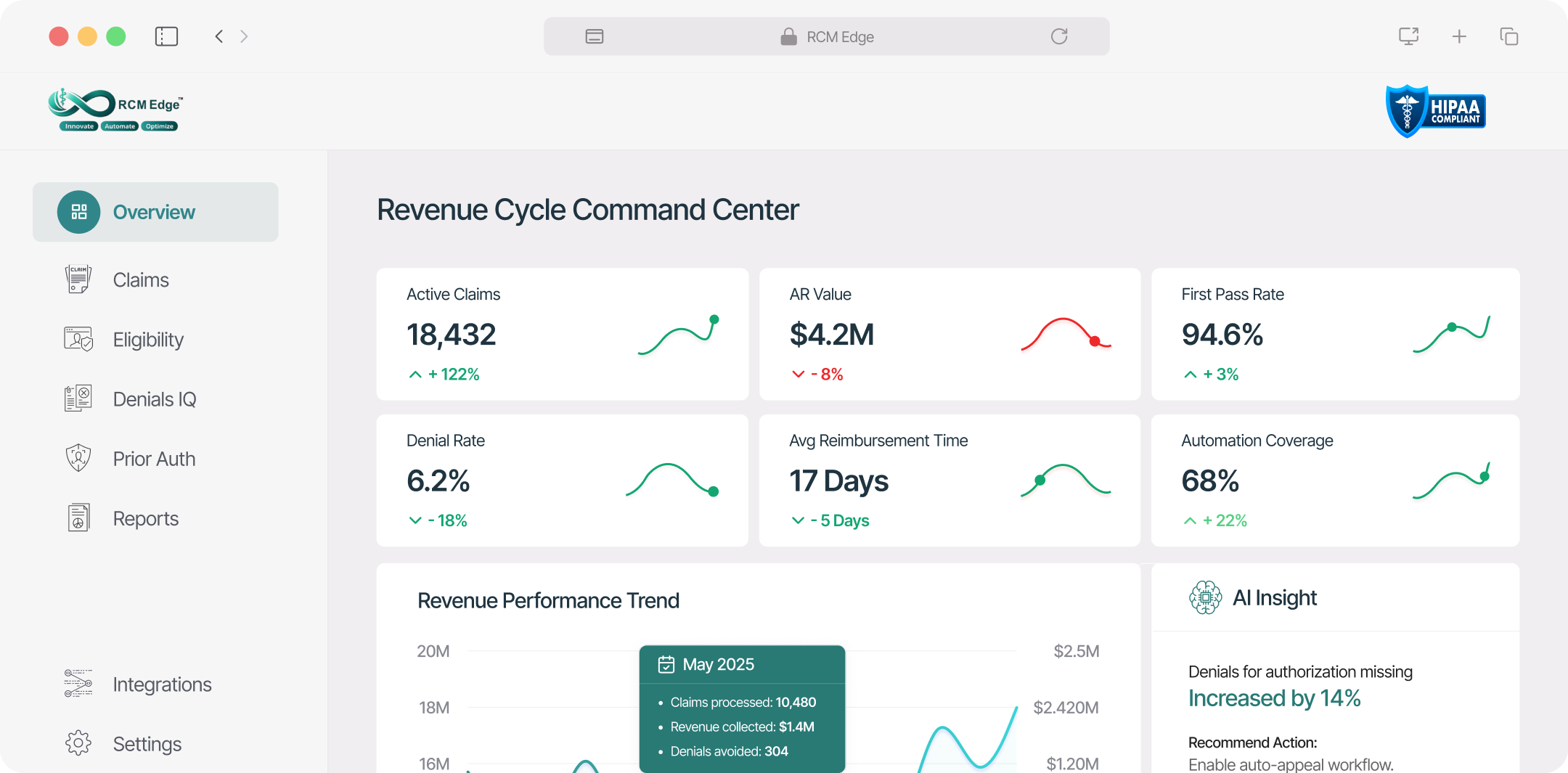
Introducing the RCM Edge Platform
A unified AI-powered revenue automation suite designed to optimize every stage of the billing lifecycle.
Full RCM Automation Suit
Introducing the RCM Edge Platform
A unified AI-powered revenue automation suite designed to optimize every stage of the billing lifecycle.
Edge Claims
Automate claim submission, validation, and payer routing with intelligent workflows that reduce rejections and accelerate reimbursements.
Edge Verify
Real-time eligibility and benefits verification powered by AI to eliminate front-end errors and improve clean claim rates.
Edge DenialsIQ
Predict, prevent, and resolve denials using machine learning insights and automated appeal intelligence with live insights.
Edge PA
Streamline prior authorization workflows with automation that reduces turnaround time and administrative burden.
Edge Insights
Gain real-time revenue intelligence with predictive analytics and performance dashboards across payers and workflows.
Unified Automation Platform
Intelligent RCM for every scale
Tailored automation workflows designed to meet the unique demands of billing companies, health systems, and specialty groups.
Maximize your operational margins by replacing labor-intensive claim follow-ups with an intelligent digital workforce. RCM Edge allows billing companies to scale their client base without a linear increase in headcount. By automating up to 70% of manual tasks , you can focus your expert staff on complex high-value appeals while our platform handles repetitive eligibility checks and status updates in real-time.
Eliminate the front-end errors that lead to revenue leakage. Designed for clinics, hospitals, and specialty groups, RCM Edge integrates directly with your existing EHR to provide instant insurance discovery and demographic verification. By ensuring clean claims from the first submission, you can significantly reduce your Days Sales Outstanding (DSO) and provide a more seamless financial experience for your patients.
Unified revenue intelligence for large-scale healthcare organizations and MSOs. Gain complete visibility across multiple tax IDs, locations, and payer networks through a single, secure dashboard. Our enterprise-ready platform is built on FHIR and HL7 standards , ensuring seamless data flow and predictive analytics that identify system-wide denial patterns before they impact your bottom line.
Payers Covered
First-Pass Rate
Reduction in DSO
Manual Task Automation
See your exact savings with RCM Edge
Adjust the sliders to match your team — your projected ROI updates instantly
Your current setup
Adjust to match your billing team
Your projected ROI
Based on avg. outcomes across 500+ billing teams
Lock in these numbers
Book a free demo — we'll validate your ROI live
Based on 2.1M+ automated transactions · 500+ billing teams measured
Try RCM Edge Risk-Free
Start Your RCM Edge 🚀 14-Day Pilot Access
See RCM Edge in action with your real claims data
RCM Automation Modules
Automate Every Step of Your Revenue Cycle
RCM Edge combines AI automation and real-time data intelligence to streamline every stage of the healthcare revenue cycle — reducing manual work while improving financial outcomes.
-
Real-time Claim Tracking
-
Eligibility & Benefits Verification
-
AI Denial Prediction
-
Prior Authorization Automation
-
Revenue Intelligence Dashboards
-
Workflow Automation Engine
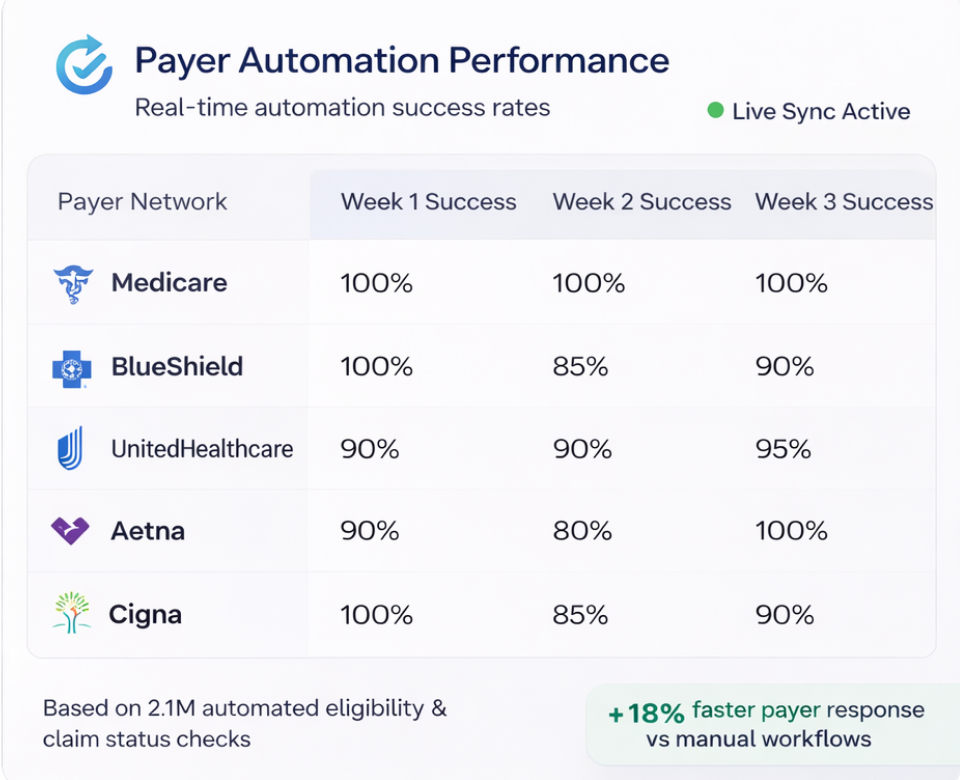
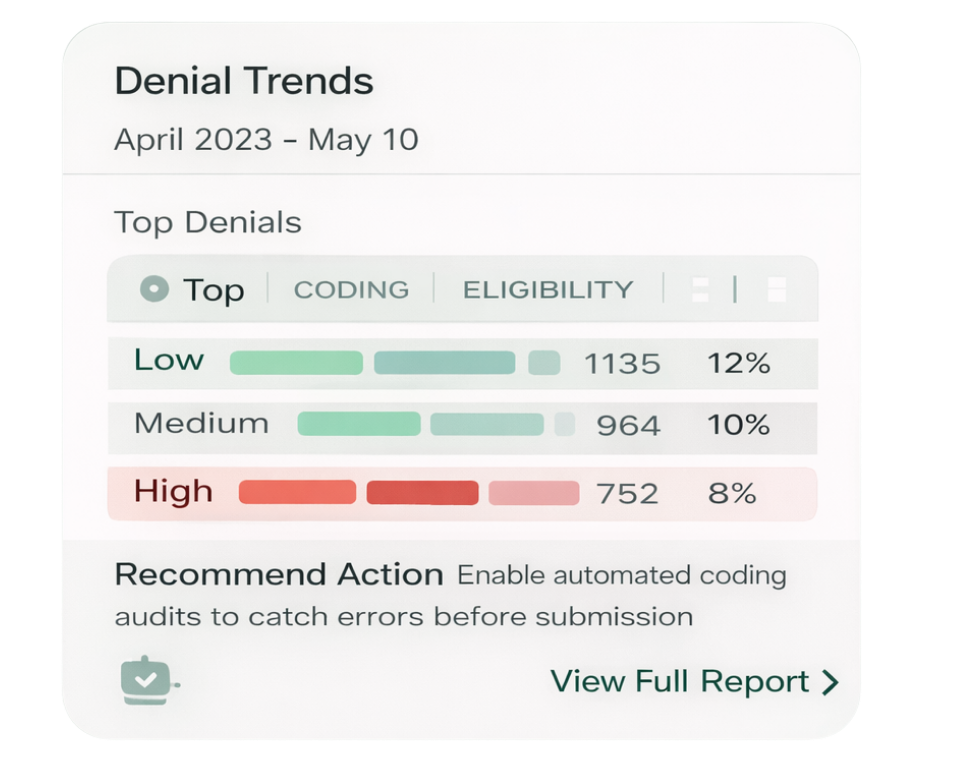
Predictive Revenue Intelligence
Predict denials, recover every dollar
Move from reactive billing to proactive revenue management. Our AI engine identifies denial patterns and root causes before they impact your cash flow.
-
Denial Prediction & Analysis
-
Root-Cause Identification
-
Payer Performance Benchmarking
-
AR Aging Optimization
-
Smart Appeal Pathways
-
Real-time Risk Scoring
Connected to 1,100+ Payers
Nationwide
RCM Edge connects your billing team to every major commercial insurer, Medicare plan, Medicaid program, and managed care organization — all through a single unified platform.
Updated continuously · FHIR · HL7 · X12 EDI
Customer Testimonials
Hear from our satisfied customers
The best way to showcase our commitment is through the experiences and stories of those who have partnered with us.
RCM Edge reduced our denial rate by over 32% in the first 90 days. The AI insights helped us identify payer patterns we were completely missing.
Brain
24/7 Medical Billing Services
Director
Increase in Clean Claim Rate in the first month.
We went from reactive billing to proactive revenue management. Our AR days dropped significantly after implementing RCM Edge automation.

Dr. Amanda Collins
North Valley Medical Group
Account Executive
Manual Hours Saved in the last 4 months
The automation coverage is a game changer. We scaled our operations without increasing headcount while improving first-pass claim rates.

Brendan Buck
RCM Velocity Solutions
Founder
Reduction in AR Days vs last year
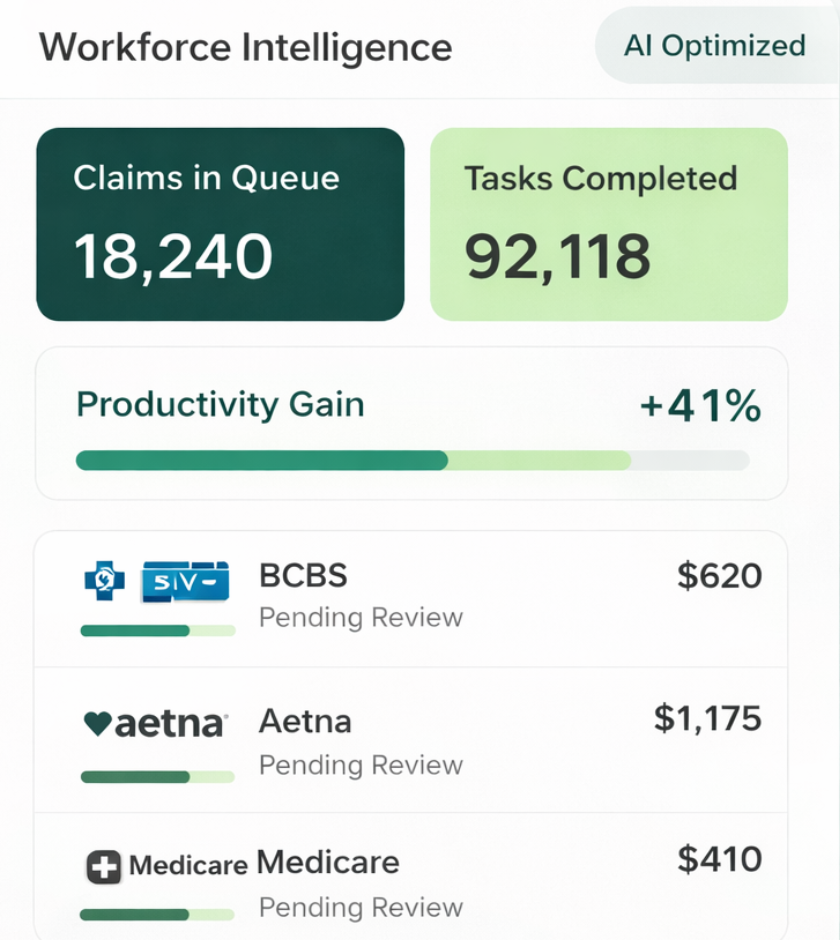
Workforce Automation
AI-Powered Workforce Automation for RCM Teams
Manage your billing team's performance effortlessly with our integrated smart-worklist and task-scheduler feature
Automatically route the highest-value claims and urgent denials to your top specialists.
Real-time monitoring of all active payer portal connections and API status.
Set-and-forget follow-up triggers for claims that remain pending beyond set thresholds.
Flexible Pricing
Flexible pricing plans. Any scale.
Whether you are an independent clinic, a growing billing company, or a national health system, we have a plan that aligns perfectly with your revenue goals.
Starter
Starter plan offers essential automation with Edge Claims and basic revenue insights — perfect for clinics and growing billing teams.
Professional
Professional plan unlocks AI-powered automation including Edge Verify, DenialsIQ, and advanced workflow intelligence for scaling revenue operations.
Enterprise
Enterprise plan delivers the full RCM Edge platform with all modules, custom integrations, and dedicated support tailored for large healthcare organizations.
Latest News
News and stories center
Explore insightful content that keeps you ahead of the curve to the pulse of what's happening.
Why Automated Eligibility Verification Is Critical for Preventing Claim Denials
Automated eligibility verification helps healthcare providers prevent claim denials and improve revenue cycle efficiency.
Manual vs Automated Claim Status Checks: Which Is Better for RCM Teams?
Manual vs automated claim status checks explained for RCM teams seeking faster reimbursements and improved billing efficiency.
How Bulk Claim Status Automation Reduces AR Days in Medical Billing
Automate bulk claim status checks to reduce AR days and accelerate medical billing reimbursements.
Launch Today
Ready to modernize your revenue cycle?
Start your RCM Edge journey today and automate claims, prevent denials, and accelerate reimbursements — without expanding your billing team.



